Constipation is one of the most common digestive issues, affecting people of all ages. It’s estimated that around 1 in 7 adults experience it, with women more commonly affected than men. While occasional constipation is normal, ongoing symptoms can be uncomfortable and disruptive. If it lasts for more than three months, it may be classed as chronic constipation and may need a more targeted approach.
What is constipation?
There is no single set definition of constipation. However, healthcare professionals often describe it as having fewer than three bowel movements per week.
That said, how often you go to the toilet is only part of the picture.
Many people think they are not constipated if they go every day, or that they are constipated if they do not. This is not always true.
What really matters is how easy it is to pass a stool and what it looks like.
For example, you might go every day but still be constipated if:
- Your stools are hard or dry
- You need to strain
- You feel like you have not fully emptied your bowels
On the other hand, going every other day can be completely normal if it feels comfortable and easy.
Common symptoms of constipation include:
- Straining when going to the toilet
- Hard, dry, or painful stools
- Feeling like your bowels have not fully emptied
- Difficulty passing stools
- Needing to use your fingers to help pass a stool
These symptoms can be uncomfortable and affect your day-to-day life.
What causes constipation?
Constipation is usually caused by a mix of factors rather than just one thing.
Some common causes include:
- Not eating enough fibre
- Not drinking enough fluids
- Sitting for long periods or not moving enough
- Ignoring the urge to go to the toilet
- Certain medications (such as iron tablets or codeine)
- Stress, anxiety, or low mood
- Weak or uncoordinated pelvic floor muscles (for example after childbirth, surgery, or injury)
Your gut bacteria may also play a role. When bacteria break down food, they produce gas. Some gases, like methane, can slow down how quickly food moves through your gut, which may lead to constipation.

How to relieve constipation naturally
If you’re wondering how to relieve constipation naturally, the good news is that simple diet and lifestyle changes are often very effective.
1. Increase fibre intake (the right way)
A high fibre diet for constipation is often the first step recommended by dietitians. Fibre helps to bulk and soften stools, making them easier to pass.
How much fibre do you need?
UK guidelines recommend:
- Adults: ~30g fibre per day
- Children: 20–25g depending on age
If your intake is low, increase fibre gradually to avoid bloating and discomfort.
Simple changes to boost your fibre intake include:
- Include more oats in your diet e.g. overnight oats, porridge oats, granola with greek yogurt or milk instead of your usual cereal, replace your digestive with a ginger or chocolate oatcake.
- Pimp up your eggs on toast with a side order of wilted spinach, pan fried mushrooms or tomatoes.
- Add extra fruit to your meals where possible e.g. fruit with your yogurt pot, add some blueberries to your salad, sliced banana to peanut butter on toast, top your bowl of porridge with berries or sliced apple.
- Research shows that eating two kiwifruit per day can improve stool frequency, consistency, and ease of passing stools. Kiwifruit contains a mix of soluble and insoluble fibre, along with natural enzymes that may help stimulate gut movement. It is often well tolerated and may cause less bloating than other fibre sources.
- Similarly 50g prunes in a recent study has been shown to help with stool consistency and frequency, however for some people prunes might exacerbate persistent bloating or wind
- Increase your intake of pulses e.g. add red lentils to your shepherds pie mix or chickpeas to your chicken curry.
- Add 1tsp ground linseeds to your yogurt or cereal and build up to 1tbsp. Ensure you take an additional 150mls water at the same time.
- Make your own chia seed jam (high in soluble fibre) by heating 1 500g bag of frozen berries with 2tbsp chia seeds and a dash of water, vanilla extract. Bring to the boil and then allow to cool. Then add to your yogurt, slice toast
- Try incorporating more wholegrain foods in your diet e.g. using brown and white rice or wholegrain seeded bread/oat based breads
- Swap your jam on toast for peanut butter on toast
- Add chopped nuts or seeds to your yogurt, bowel cereal or sprinkle some over your salads
- Next time you reach for a bag of crisps try grabbing a handful of nuts instead
2. Consider psyllium husk (a proven fibre supplement)
If you struggle to meet your fibre needs through food alone, psyllium husk for constipation is one of the most evidence-based options.
Psyllium is a soluble fibre that forms a gel in the gut, helping to:
- Soften stools
- Improve stool consistency
- Support regular bowel movements
It is often recommended as a first-line supplement for constipation and is generally well tolerated.
How to take psyllium husk:
- Start with a small dose and increase gradually e.g. ½ teaspoon to 1tsp
- Always take with plenty of water
- Take consistently for best results
3. Stay hydrated
Fluid intake plays a key role in preventing and relieving constipation. Without enough fluid, stools can become hard and difficult to pass.
How much should you drink?
- Under 60 years: ~35ml per kg body weight per day
- Over 60 years: ~30ml per kg per day
Best drinks for constipation
- Water
- Herbal teas
- Milk or dairy alternatives
- Diluted squash
- Small amounts of fruit juice (limit to ~150ml if prone to bloating)
Caffeinated drinks like tea and coffee can be included, but try to limit to around 2 cups per day if you are sensitive.
⚠️ When increasing fibre (especially oats, seeds, or psyllium), it is essential to increase your fluid intake as well.
4. Eat regular meals
Skipping meals can worsen constipation.
Eating triggers the gastrocolic reflex, which stimulates movement in the digestive tract. This helps promote bowel movements after eating.
To support regular bowel habits:
- Aim for three meals per day
- Avoid long gaps without food
- Include fibre at each meal
5. Move your body daily
Regular movement helps stimulate bowel activity and supports overall gut health.
Exercise can:
- Increase gut motility
- Reduce transit time
- Help manage stress (which is linked to constipation)
You don’t need intense workouts—simple daily movement is enough:
- Walking
- Taking the stairs
- Yoga or stretching
- Any activity you enjoy
Reducing sedentary time is just as important as structured exercise.
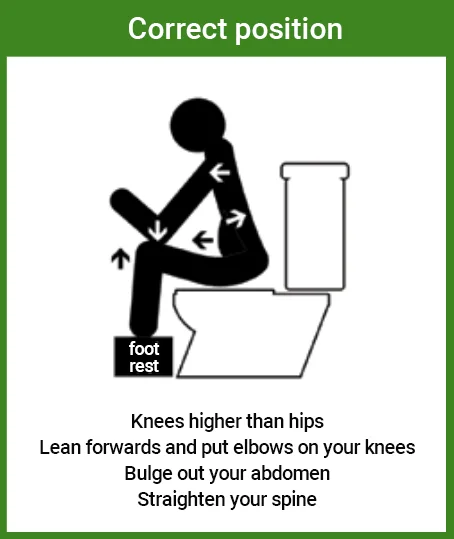
Prioritise your pooping position!
How and when we poop is important to support a successful evacuation as incomplete evacuation can contribute to constipation and cramping.
Key things to remember when sitting on the toilet are to put your feet up on a stool to ensure your knees are higher than your hips, lean forward slightly resting your forearms on your thighs and take some deep abdominal breaths.
Also try not to put off going to the toilet when you feel the urge as “holding your poo in” and delaying your bowel movement can contribute to constipation. Water is reabsorbed back into the body in the colon so the longer the stool remains, the more water is reabsorbed resulting in a hard drier and likely difficult stool to pass.
Key takeaways: simple tips to prevent constipation
Aim for 30g fibre per day
Include foods like kiwifruit and oats regularly
Consider psyllium husk if needed
Drink enough fluids daily
Eat regular meals
Stay physically active
When to seek medical advice
If constipation persists despite these changes, or if you experience symptoms such as unexplained weight loss, blood in your stool, or persistent pain, it is important to speak to your GP.
Lets Talk
No one likes talking about poo and bowel habits (unless you are a gastro dietitian like me!).. However if you are suffering with constipation and would like more help to manage your bowel habits contact me and I would love to help you.
Alternatively this constipation guide from The Guts Charity is a great read: Constipation